Common Cardiac Conditions
- ASD Surgery in Delhi
- VSD Surgery in Children in Delhi
- Best PDA Surgery in Delhi
- Coarctation of Aorta Treatment in Delhi
- Aortic Stenosis Treatment in Delhi
- Pulmonary Stenosis
- Atrio-Ventricular Septal Defect (AVSD/AVCD)
- RSOV Treatment in Delhi
- Eisenmenger Syndrome/ Complex
- Tetralogy of Fallot Treatment
- Transposition of Great Arteries (d-TGA)
- Total anomalous pulmonary venous connection treatment in Delhi
- Truncus Arteriosus
- Tricuspid Atresia
- Double Outlet Ventricle
- Congenitally Corrected Transposition of great vessels in Delhi
- Ebstein’s Anomaly
- Pulmonart Atresia (PA) Without VSD/Intact Septum
- Pulmonart Atresia (PA) with VSD
- Hypoplastic Left Heart Syndrome
- Stenosis of Pulmonary Artery Branches
- Patent Foramen Ovale (PFO)
- AP Window Device Closure
- Vascular Rings
- Interrupted Aortic Arch (IAA)
- Bicuspid Aortic Valve Treatment
- SVT treatment in children
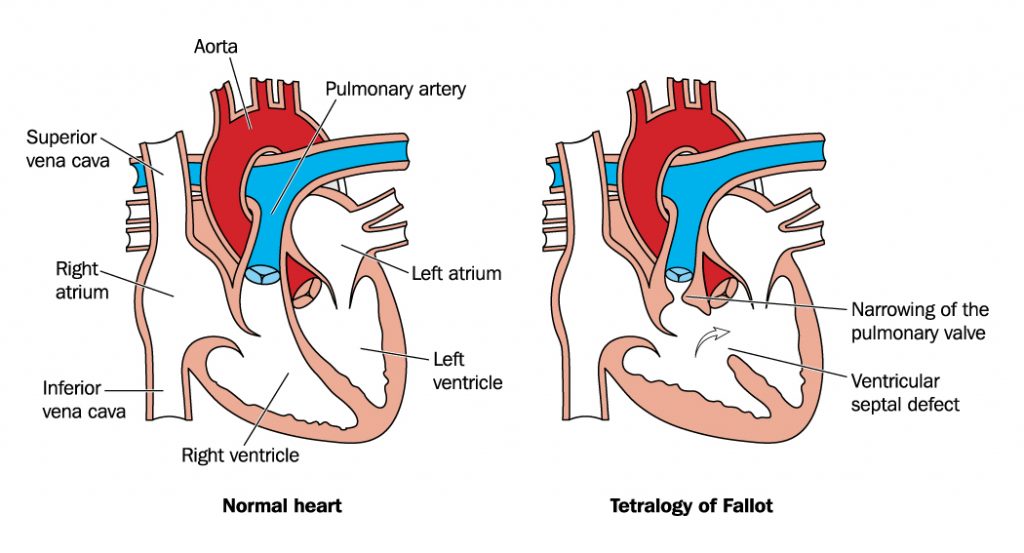
Tetralogy of Fallot In Children
Tetralogy of Fallot (TOF) is a cyanotic congenital heart disease. It is the commonest cyanotic congenital heart defect (C-CHD).
This disease consists of large hole in lower part of the heart known as Ventricular septal defect (VSD)along with severe narrowing in outflow tract of right sided ventricle known as pulmonary stenosis (VSD and PS) with anterior mal-alignment of conal septum.
Pulmonary stenosis can be either infundibular/valvular/supravalvular pulmonary stenosis.
With long standing pulmonary stenosis, right sided ventricle muscles got thickened (Right ventricle hypertrophy; RVH). In severe form of TOF, there can be total obstruction of right ventricle outflow (Pulmonary Atresia).
Additional heart diseases that can be associated with TOF can be additional VSDs, atrial septal defect(ASD), abnormal coronary arteries etc.
Majority of children who are affected with Tetralogy of Fallot (TOF) are associated with chromosomal abnormalities, such as 22q11 deletion syndrome (Digeorge Syndrome).
Due to pulmonary stenosis, there will be decreased blood supply to the lungs that leads to bluish discoloration of lips and fingers (cyanosis) due to flow of poorly oxygenated blood to the body parts through the VSD. Severity of cyanosis depends on the severity of pulmonary stenosis. Cyanosis can be seen on examination and if not visible clinically, can be assessed by saturation monitoring (SPO2).
Tetralogy of Fallot Symptoms (TOF symptoms)
Tetralogy of Fallot (TOF) if severe, then can be easily diagnosed in first few days of life either due to cyanosis or due to abnormal heart sound heard by a neonatologist.
But, TOF baby (newborns) generally do not have cyanosis early in life due to presence of patent ductus arteriosus (PDA) at birth that supplies additional blood to the lungs. But as soon as PDA closes and pulmonary stenosis is severe, baby can be extremely blue and breathing can be rapid and labored.
When pulmonary stenosis is very severe then on crying, child may get “cyanotic spell” that is characterized by severe cyanosis with rapid breathing (air hunger). It sometimes can lead to seizures and loss of consciousness.
The most common sign in children with TOF is cyanosis – a tint of purple or blue on the lips, skin, and fingernails.
Other symptoms/signs to look out for include –
- Irritability
- Clubbing of toes and fingers
- Poor weight gain
- A heart murmur
Complications of TOF-
Child may get following with TOF:
- Cyanosis deteriorating over a period of time
- Cyanotic spells (Tet spell)
- Seizures/loss of consciousness
- Infective endocarditis (IE)– an infection of the lining of your heart
- Irregular heartbeat or arrhythmia
Diagnosis of TOF (Children Tetralogy of Fallot)
Children TOF can be easily diagnosed by doing “Fetal Echocardiogram”. Fetal Echocardiogram needs to be done ideally between 18-24 weeks of gestation preferably between 18-20 weeks of gestation.
Pink TOF: When there is mild pulmonary stenosis then child may not have cyanosis even with large VSD and PS, this is known as Pink TOF. These children TOF are suspected by murmur on examination and followed by children echocardiogram evaluation.
Severely cyanosed TOF affected child can be suspected on clinical examination by seeing the cyanosis and by hearing murmur in chest.
Other tests that can be supportive in making the diagnosis are ECG, chest X-ray.
Sometimes CT angio of heart needs to be done for defining the structure of heart when echocardiogram is inconclusive. Occasionally especially in older children or adolescents, Cardiac cath angiography has to be done when CT angio is less desirable.
Children TOF Treatment
Once TOF is diagnosed, treatment is decided by symptoms of the baby. If baby is very blue with low oxygen content in the body then immediate surgery or cardiac intervention is required to improve the oxygen content in the body including the brain. Treatment is mainly done when saturation is less than 75% (TOF surgery indication).
If pulmonary atresia is there (severest form of TOF), then newborn may require IV medications in the form of prostaglanding infusion (PGE1) for patent ductus arteriosus open so that blood supply to the lungs maintained. These babies will require immediate surgical intervention in the neonatal period in the form of Blalock-Taussig shunt (BT shunt) or cardiac intervention in the form of PDA stenting (Patent Ductus Arteriosus stenting) depending on baby weight and cardiac anatomy.
In case of severe RVOT obstruction and low weight of the baby, we can plan stenting of right ventriculat outflow tract (RVOT/right ventricular outflow stenting) in cath lab by angiography (When BT shunt is high risk).
Intracardiac repair in the form of complete TOF repair is generally done between 6-9 months of age (preferably before one year of age; TOF surgery age) even if child is asymptomatic.
Definite treatment for children TOF is only surgical (TOF Surgery)
By surgery, we close VSD by an artificial patch and relieve the RVOT obstruction (PS) by resection of muscles in outflow tract.
If coronary arteries are having abnormal course and crossing the right ventricular outflow tract then we need to put an artificial conduit in outflow tract instead of muscle resection of outflow tract (pulmonary artery conduit).
Hypertrophy of right ventricle decreases gradually over a time period.
Most children do well after complete surgery. Follow-up with Pediatric Cardiologist is required to ensure well being of the child.
Success rate after TOF surgery
Now a day, success rate after TOF surgery is high with approximately success rate of 98-99%. It took around 1-2 hours for TOF surgery (TOF surgery time).
How to treat children cyanotic Spell?
- First and foremost is to keep the child calm.
- We should keep the child in knee-chest position by folding the legs into abdomen and keeping the neck in flexed position.
- Immediate IV cannula, followed by rapid saline bolus and IV ketamine and subcuatneous morphine to be given.
- Oxygen
- IV metoprolol infusion
- Sadium Bicabonate IV bolus if required
- If not responding then ventilate the child
Follow-up treatment after TOF repair/TOF surgery complications
In modern scenario, survival after TOF repair has been improved significantly. The results can be sub-optimal when pulmonary arteries (lung vessels) are very small in size or when lung vessels are not developed and lungs are getting its blood supply by abnormal collaterals.
Patient may require treatment for cardiac rhythm disorders in the form of pacemakers, can require artificial pulmonary valve implantation when pulmonary valve is sacrificed during repair of TOF.
Sometimes, patient can develop restenosis of RV outflow tract and for that re surgery to be done.
Occasionally, left sided pulmonary artery is narrowed and even after increasing its size by surgery, size does not increase then we can palliate the artery by putting a stent across it so that its size can be increased, known as LPA stenting or pulmonary artery stenting.
TOF in adults and adolescents
Generally, we see adults after repair of TOF in their childhood.
Unfortunately, the majority do have issues due to sacrifice of pulmonary valve during complete repair known as “pulmonary regurgitation.” This can leads to increase in size of right ventricle and can also leads to limitation in physical activities as well as leads to arrythmias.
So, adults should have a regular follow-up with a paediatric cardiologist throughout their life.
Fortunately, if these artificial valves fail, now a day, we can replace the valve by transcatheter technique by angiography (Pulmonary Valve Replacement; PVR).
Looking for Tetralogy of Fallot Treatment in Delhi? Contact - Dr. Gaurav Agrawal
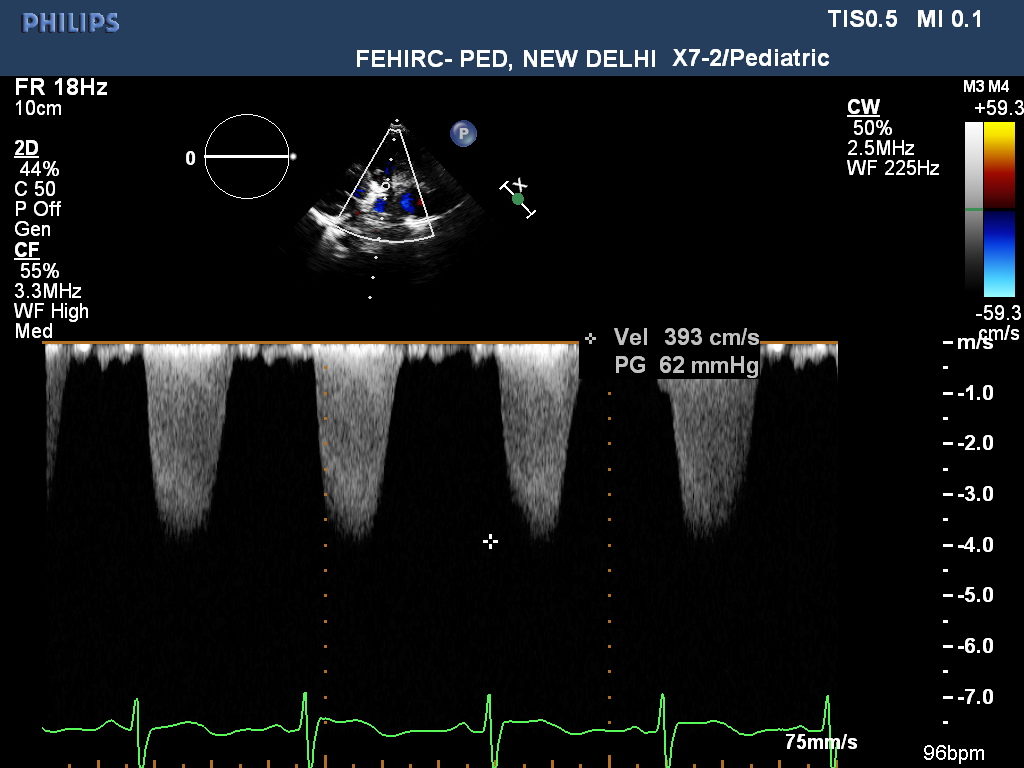
TOF
TOF with large VSD
TOF with Pulmonary Stenosis