Common Cardiac Conditions
- ASD Surgery in Delhi
- VSD Surgery in Children in Delhi
- Best PDA Surgery in Delhi
- Coarctation of Aorta Treatment in Delhi
- Aortic Stenosis Treatment in Delhi
- Pulmonary Stenosis
- Atrio-Ventricular Septal Defect (AVSD/AVCD)
- RSOV Treatment in Delhi
- Eisenmenger Syndrome/ Complex
- Tetralogy of Fallot Treatment
- Transposition of Great Arteries (d-TGA)
- Total anomalous pulmonary venous connection treatment in Delhi
- Truncus Arteriosus
- Tricuspid Atresia
- Double Outlet Ventricle
- Congenitally Corrected Transposition of great vessels in Delhi
- Ebstein’s Anomaly
- Pulmonart Atresia (PA) Without VSD/Intact Septum
- Pulmonart Atresia (PA) with VSD
- Hypoplastic Left Heart Syndrome
- Stenosis of Pulmonary Artery Branches
- Patent Foramen Ovale (PFO)
- AP Window Device Closure
- Vascular Rings
- Interrupted Aortic Arch (IAA)
- Bicuspid Aortic Valve Treatment
- SVT treatment in children
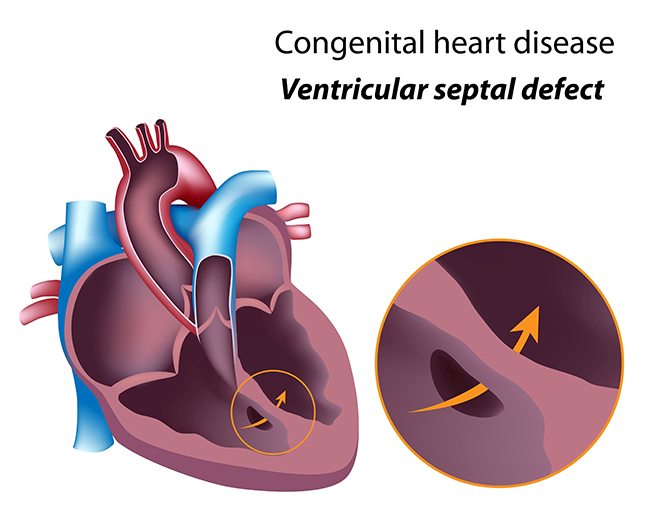
Ventricular Septal Defect (VSD)
VSD (a hole in the heart) refers to a congenital heart disease (CHD) where a hole is formed in the ventricle septum i.e. wall that separates two lower chambers of the heart.
As a result of this, blood from the left portion of the heart (left ventricle) crosses this hole and goes to right-sided heart that results in overflow of blood to the lungs.
Ventricular septal defect is one of the commonest child heart diseases that are seen at birth, but adults too may suffer from it following an acute heart attack (Ventricular septal defect in Adults, Post Infarction ventricular septal defect, Post MI VSD).
What is the cause of Ventricular Septal Defect (VSD causes)?
Congenital ventricular septal defect (congenital VSD) occurs during development of fetus heart. The heart develops from a huge tube, dividing into sections that, in turn, will become the chambers, walls and vessels of the heart. If something goes wrong during this process, a hole can develop in the ventricular septum.
Sometimes, VSD may be caused due to genetic and environmental factors. For instance, if you have a family history of genetic conditions like Down syndrome or congenital heart diseases, then your child may be at risk of developing a Ventricular Septal Defect.
Symptoms of ventricular septal defect:
The signs and symptoms of VSD vary depending on the size of the VSD. If the hole is small, child may be asymptotic. Children or young adults with small VSD only show signs of a heart murmur (Ventricular Septal Defect murmur) that is detected by their family physician.
A medium or large sized hole is likely to exhibit the following noticeable symptoms in children due to VSD:
- Rapid breathing/Breathlessness
- Poor weight gain/ Failure to thrive
- Poor feeding
- Tiredness and fatigue
- Excessive sweating
- Inability to engage in physical activities
- An enlarged heart
- A tint of blue on the lips, fingernails, and skin in late stages of large VSD (Eisenmenger VSD)
These symptoms indicate that the VSD will most likely not close by itself, and therefore, require urgent treatment (VSD treatment).
If left untreated, Ventricular Septal Defect may lead to further complications such as pulmonary hypertension, endocarditis, or Eisenmenger complex like situation.
How VSD is diagnosed (Ventricular Septal Defect diagnosis)?
Pre-natal testing in the form of foetal echocardiogram can reveal ventricular septal defect during pregnancy state (even before delivery of the child). It helps in planning of delivery of the child for timely initiation of treatment as soon as newborn is delivered.
Usually, VSD is detected within the first few weeks after the birth of the child during a routine check-up. The doctor can tell if your child has a hole in the heart by hearing a heart murmur, as oxygen-rich blood passes between the two ventricles.
Suspecting VSD, your doctor may refer you to a paediatric cardiologist, who will then perform a physical examination on your child, taking his/her medical history in consideration.
The following tools are used to confirm the diagnosis –
- X-ray of the chest
- Electrocardiogram or ECG
Most importantly by doing a Pediatric Echocardiogram: this is done from the child's chest, a non-invasive modality with no pain to the child
What is the treatment of VSD?
Treatment of VSD depends on the size of the hole, and the age and weight of the child.
A small VSD with no significant symptoms mostly will require only follow-up. The child can do his/her activities without much fear.
Moderately sized VSD children are having poor weight gain and show signs of heart failure but less as compared to large VSD. These VSD needs to be followed up to 9-12 months of age and needs to close. The method of closure of moderate sized VSD depends on its location and size of VSD. Majority of moderate sized VSD can be closed by using a device in cath lab angiographically (VSD device closure non-surgically) or else by doing open heart surgery.
In a case of large VSD: Child shows signs of heart failure or in respiratory distress then first medical therapy in the form of diuretics are prescribed for decreasing the signs of heart failure. Then VSD surgical closure is advised preferably between 3-6 months of age.
Heart Surgery – This involves making an incision in the chest wall and maintaining circulation with the help of a lung-heart machine while closing the hole. The surgeon may either seam the hole or stitch a patch of material over it. The heart tissue will eventually heal over the stitches or patches. In about six months, the tissue will cover the hole completely.
Another treatment option is cardiac catheterization.
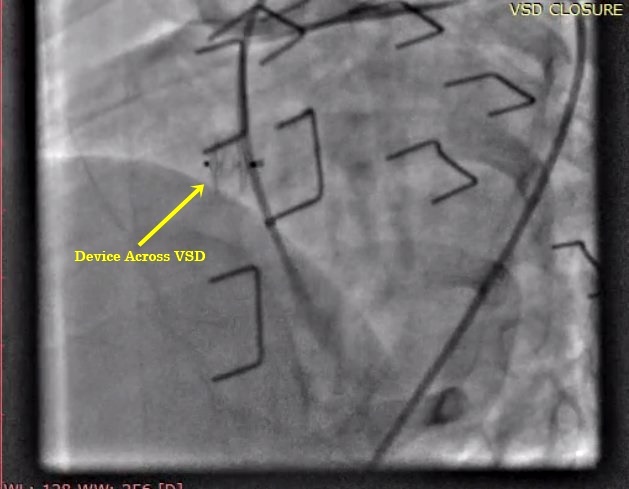
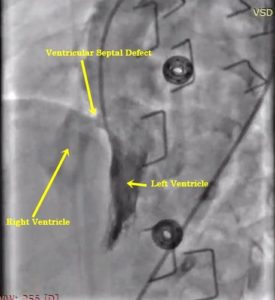
Non-surgical closure of VSD
The cardiologist inserts a catheter into the blood vessel in child legs that reach up to the heart. He/she then guides the tube to make measurements of blood pressure, blood flow, and level of oxygen in the chambers of the heart. A special implant known as a device is placed into the septal hole (VSD). The device flattens against the septum on both the sides to permanently heal and close the VSD (VSD device closure).
Risks associated with VSD closure by angiograpy
Although VSD Device closure is a safe procedure but may be associated with few risks depending on the location of VSD. These may include heart block or rhythm disturbances (transient or permanent) requiring pacemaker, new onset heart valve leaks etc.
Minor adverse events may be in the form of blood collection in groin although very rare; device can embolized requiring surgical removal and loss of pulse in the limb etc.
Adults with Ventricular spetal defect (VSD)
Usually treatment is recommended to prevent heart and lung problems. Adults may have VSD since birth or may have VSDs after ischemia to muscles of (Post MI VSD).
Medical Follow-up
Regular follow-up is required with VSD if not closed. If VSD is not associated with other congenital heart diseases and there is no evidence of pulmonary arterial hypertension then we need not to follow regularly after one year of surgical closure of VSD.
Drug treatment is only required when child is in heart failure or having pulmonary arterial hypertension.
Infective Endocarditis prevention
Unrepaired VSD does not require prophylaxis for VSD. There is mild risk of having infective endocarditis with VSD so child shall receive antibiotics before certain dental procedures for a period of time after VSD repair.
Activity Restrictions with VSD
In case of small VSD, or if the VSD has been closed with surgery, there is no need of any activity restrictions if not associated with other form of heart diseases.
Pregnancy and VSD
Pregnancy after closure of VSD with no pulmonary arterial hypertension is having very low risk.
However pregnancy is contraindicated with Eisenmenger VSDs.
ReDo surgery is required after VSD closure?
Rarely, may need if there is significant residual leak after surgery.
Success rate after VSD surgery
There is very good success rate after surgical closure of VSD if not associated with other heart problems.
Looking for VSD Surgery in Children in Delhi? Contact - Dr. Gaurav Agrawal
VSD
VSD